How to save manpower when doing head repositioning in prone position?
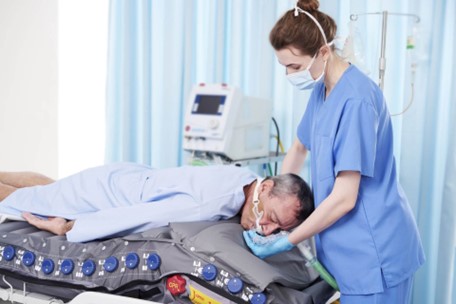
Simplifying Head Repositioning with Optima Prone Minimizes Risks for Caregivers and Patients.
The need for head repositioning in the prone position every two hours complicates ICU management.
Prone position has been frequently used in the intensive care units to improve the prognosis in patients with acute respiratory distress syndrome (ARDS).
Regarding the American journal of respiratory and critical care medicine (AJRCCM) and Critical Care Nurse practice guideline, requiring a team of 5 caregivers to complete supine and prone maneuvers and a team of 3 caregivers to reposition the patient’s head every 2-4 hours, with therapy lasting 12 to 16 hours1,2.
The current situation: frequent labor-intensive patient handling maneuvers, significantly increasing harm to caregivers.
Lifting a patient's shoulder for a head repositioning maneuver requires a team of 3 caregivers every 2-4 hours. This is a labor-intensive procedure and potentially causes harm to caregivers. Head repositioning is a highly complex maneuver, requiring caregivers to simultaneously hold and turn the patient's head while stabilizing tubes to prevent unintended extubation or obstructions.
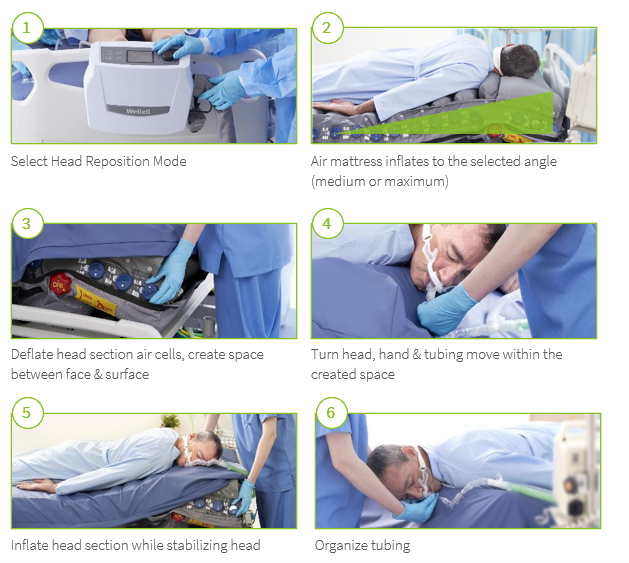
- Related Article:
Repositioning Patients to Prevent Pressure Injuries
1.
Lauren
MorataKathleen
VollmanJennifer
RechterJill Cox;
Manual Prone Positioning in Adults: Reducing the Risk of Harm Through
Evidence-Based Practices. Crit Care Nurse 1 February 2023; 43 (1): 59–66.
doi: https://doi.org/10.4037/ccn2023174
2.
Fan, Eddy et al. “An
Official American Thoracic Society/European Society of Intensive Care Medicine/Society
of Critical Care Medicine Clinical Practice Guideline: Mechanical Ventilation in Adult
Patients with Acute Respiratory Distress Syndrome.” American journal of
respiratory and critical care medicine vol. 195,9 (2017): 1253-1263.
doi:10.1164/rccm.201703-0548ST

