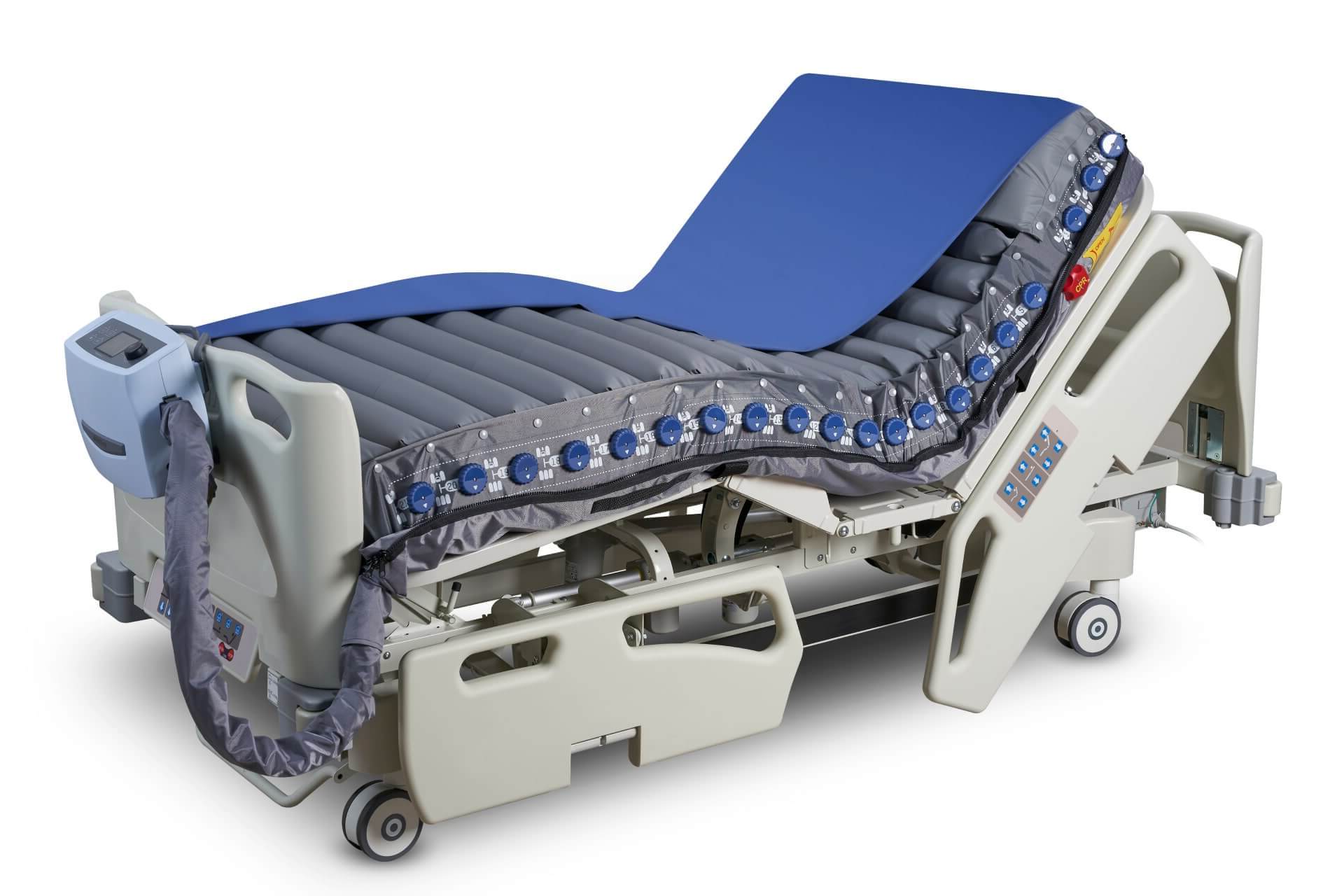
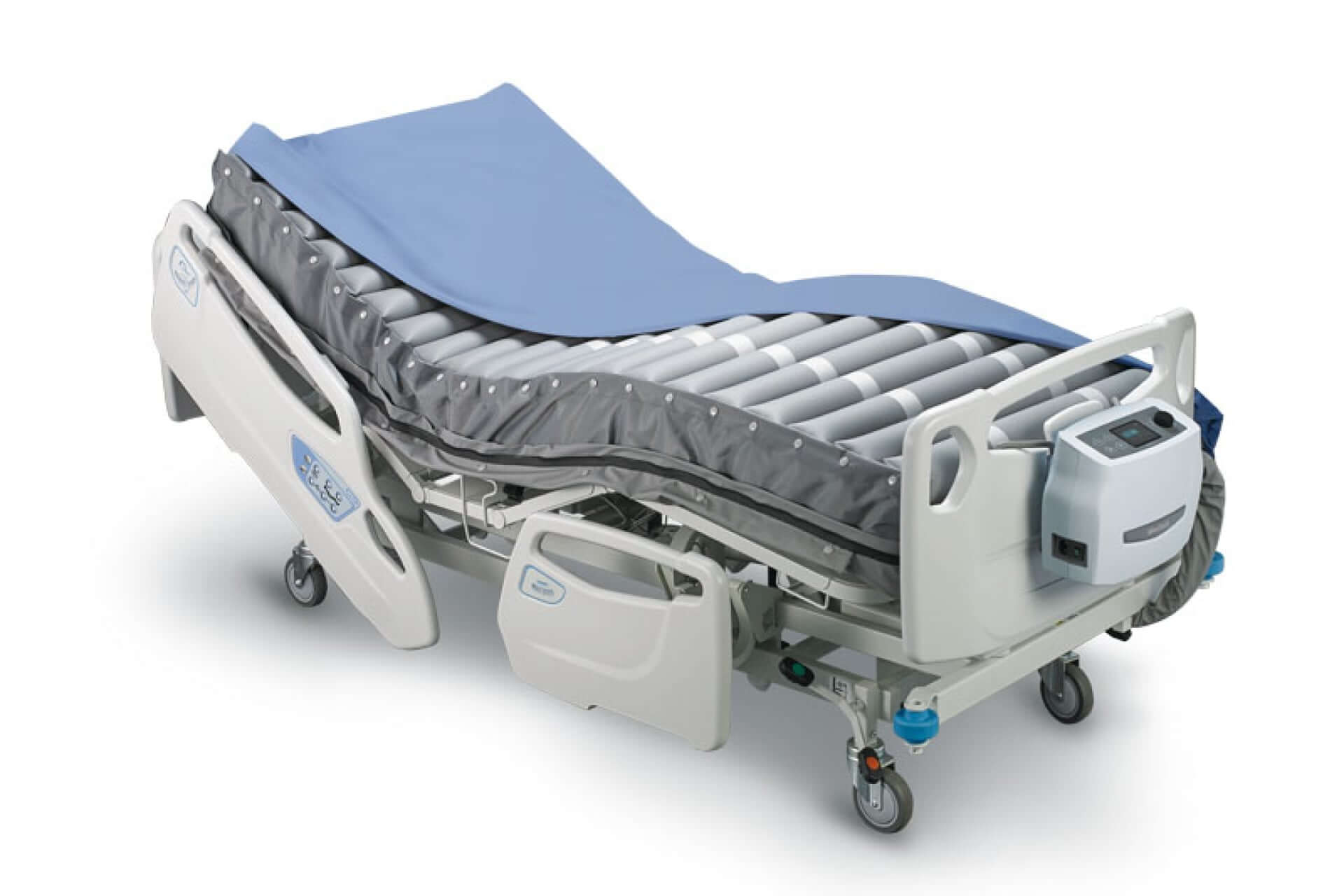
Optima Turn
Lateral Rotation MattressFor High to Very High Risk
Automated Lateral Rotational Pressure Relief Solution -Improving repositioning feasibility and patient comfort.
Abbreviation: PI, pressure injury
Optima Turn is a s pressure relief support surface designed to enhance pressure injury prevention and reduce caregiver workload for repositioning.
According to international clinical guidelines, patients should be repositioned every 2-4 hours to prevent PI. The EPUAP/NPUAP/PPPIA guideline recommends that turning patients regularly to the 30° lateral position reduces the incidence of PI compared to 90° lateral position. However, this frequent repositioning creates a labor-intensive workflow, leading to 61.5% of nurses experiencing back pain from moving or lifting patients in bed.1,2
The thoughtful user experience design of Optima Turn has the turning function embedded with alternating to provide optimal pressure relieving, also minimizing changes to existing workflows while providing greater efficiency and comfort for both patients and caregivers.
-
Clinical rationale for using Optima Turn:
Repositioning Patients to Prevent Pressure Injuries
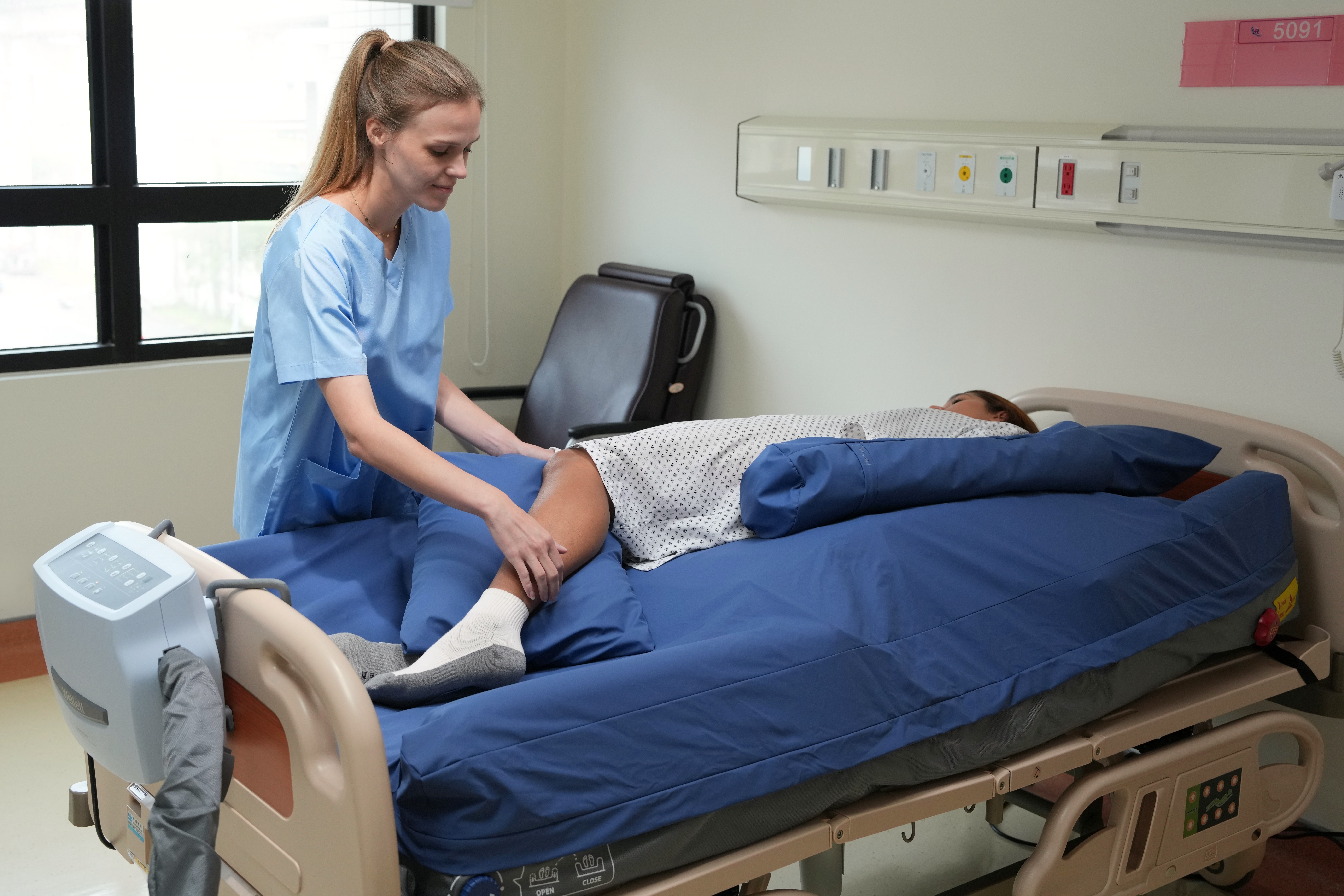
Consistent Repositioning Quality
Ensure consistent repositioning quality, improve PI prevention, and further reduce caregiver workload. Automatic turning mode reduces the number of caregivers required from 2–3 to just 1, minimizing patient handling complexity the variability in caregiving practices.
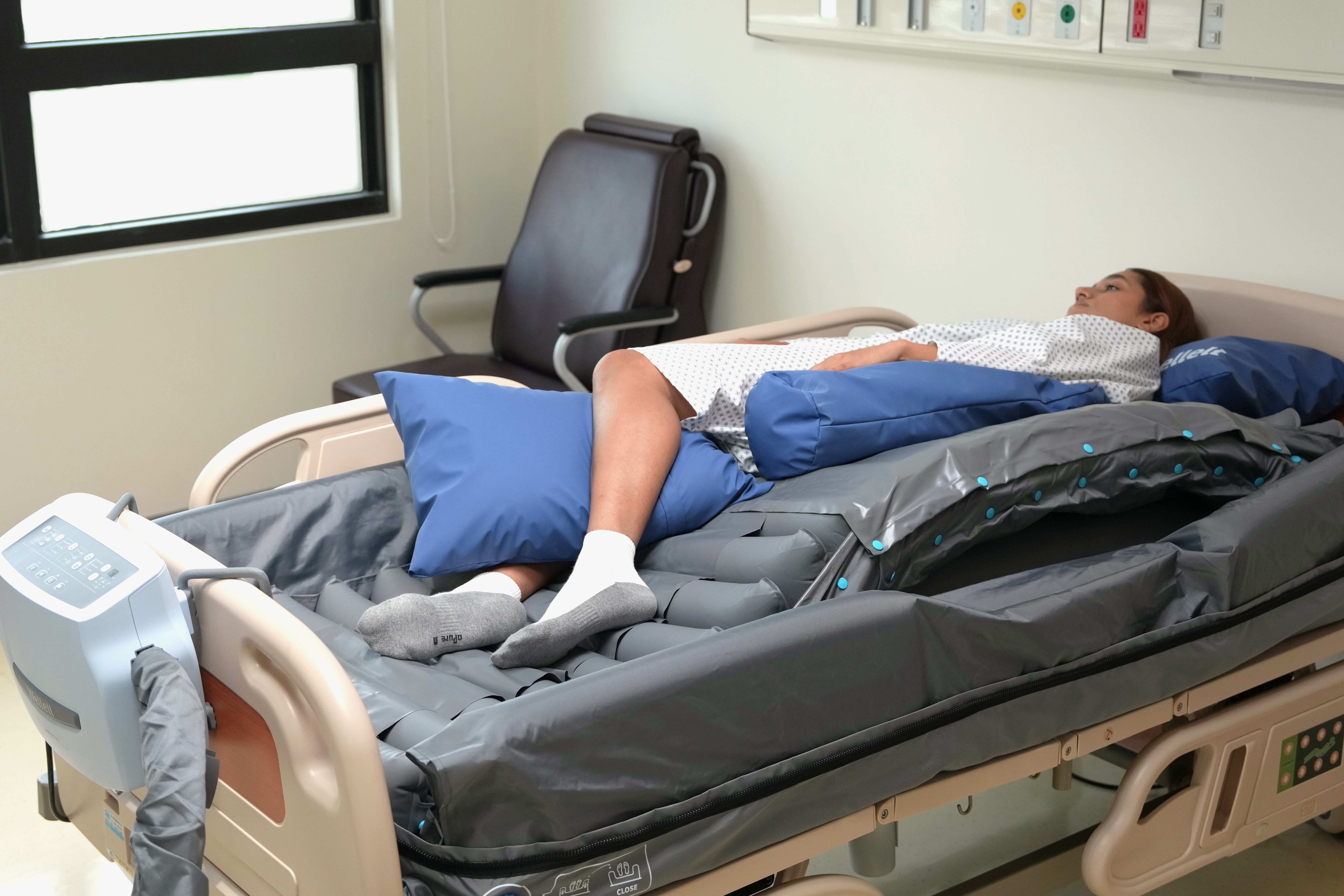
Safe and Effective Repositioning
Provide a safer and more effective repositioning solution. System enables alternating during turning for superior pressure relief, while bolsters design can provide a safer turning function that would seamlessly fit in caregiver's daily workflow. Lower mid-section of side bolster design creates an exist for drainage tubes.

Optimal Pressure Relief
Effective pressure relief by automated lateral rotation. Through the alternating air cells matching the bodyline with 30° of turning, the pressure mapping shows the ideal pressure redistribution is achieved.

Personalize Heel Relief Care
Accommodate pressure relief care for different body types by deflating individual air cells at the heels to maintain zero-pressure heel relief, minimizing the patient's risk of developing pressure injuries and prolonging the length of treatment.
| Optima Turn | ||
|---|---|---|
| Mattress Dimension (L x W x H ) | 78.7 x 33.5-35.4 x 10 in | 2000 x 850-900 x 254 mm |
| Mattress Weight | 27.5 lb | 12.5 kg |
| Maximum Patient Weight | 396 lb | 180 kg |
| Pump Dimension (L x W x H ) | 13.4 x 6.5 x 10.2 in | 341 x 165 x 260 mm |
| Supply Voltage | 110-240 V / 50-60 Hz |
|

Consistent Repositioning Quality
Ensure consistent repositioning quality, improve PI prevention, and further reduce caregiver workload. Automatic turning mode reduces the number of caregivers required from 2–3 to just 1, minimizing patient handling complexity the variability in caregiving practices.

Safe and Effective Repositioning
Provide a safer and more effective repositioning solution. System enables alternating during turning for superior pressure relief, while bolsters design can provide a safer turning function that would seamlessly fit in caregiver's daily workflow. Lower mid-section of side bolster design creates an exist for drainage tubes.

Optimal Pressure Relief
Effective pressure relief by automated lateral rotation. Through the alternating air cells matching the bodyline with 30° of turning, the pressure mapping shows the ideal pressure redistribution is achieved.

Personalize Heel Relief Care
Accommodate pressure relief care for different body types by deflating individual air cells at the heels to maintain zero-pressure heel relief, minimizing the patient's risk of developing pressure injuries and prolonging the length of treatment.
Automating caregivers’ workflow and improving pressure injuries prevention and long-term patient care.

Guideline recommends 30° over 90° repositioning.
Clinical Guideline recommends regularly turning patients to 30° lateral position to reduce pressure injury incidences, compared with usual care (90°). Repositioning to 30° every 3 hours reduces early-stage PI occurrence by 67% (compared to 90° every 6 hours).3
- Save caregiver's time.
- Relieve pressure on the hips, sacrum, greater trochanters and heels.
- Provide comfort and stability.
- Reduce caregivers' exposure to potential harm from intensive patient handlings, such as lifting and resituating patients.
- Help reposition patients and increase their mobility.
- Customize pressure settings based on the patient's needs.
- Continue pressure relief care during transports and events where immediate power is unavailable.
- Promote active recovery with inflated seating which provides support and stability and prevents patients from bottoming out.
The side bolsters protect patients from pressing directly against the side railing and sliding off the mattress. The firmness of these air cells also provides additional comfort for the patient's side when in turn.
Optima Turn's mattress provides continuous alternating pressure relief, and the side bolsters protect patients from pressing against the railings while providing comfort. In addition, individual deflatable air cells allow caregivers to customize heel relief care. For more posture support, Turn minimizes the caregivers' labour in lifting the patient to place foam or pillows as needed quickly.
- Unconscious
- Bedbound and immobilized
- Medium to high risk of pressure injures, especially on the scapulae (back shoulder area) and greater trochanters (hip side area)
ICU, GICU, NICU, Neurosurgery and Neurology, and long-term care facilities.
After powering on Optima Turn, the air cells will automatically inflate to their maximum firmness. Once the inflation process is complete, the caregiver can choose between continuous low pressure or alternating pressure modes based on the patient's needs. The pump will automatically switch to the alternating pressure mode if a mode is not selected within the first 10 minutes after the initial inflation process.
It takes 3-5 minutes to change from left to right turn and vice versa. The patient's BMI (body mass index) and body contour will influence turning duration, with heavier patients taking longer to change between turns. The dwell time starts counting when the turn reaches the selected degrees immediately.
No. In turn, the alternating pressure mode is part of the default mode and cannot be deactivated.
All air cells are made from Thermoplastic Polyurethanes (TPU). It is highly resistant to breaking down when in contact with water (hydrolysis), soft to touch, and minimizes friction and noise during patient movements.
Reference
- Courtney H. Lyder; Elizabeth A. Ayello. Patient Safety and Quality: An Evidence-Based Handbook for Nurses -Chapter 12 Pressure Ulcers: A Patient Safety Issue.
- Owen B. D. (1989). The magnitude of low-back problem in nursing. Western journal of nursing research, 11(2), 234–242.
- European Pressure Ulcer Advisory Panel, National Pressure Injury Advisory Panel and Pan Pacific Pressure Injury Alliance. Prevention and Treatment of Pressure Ulcers/Injuries: Clinical Practice Guideline. The International Guideline. Emily Haesler (Ed.). EPUAP/NPIAP/PPPIA; 2019.